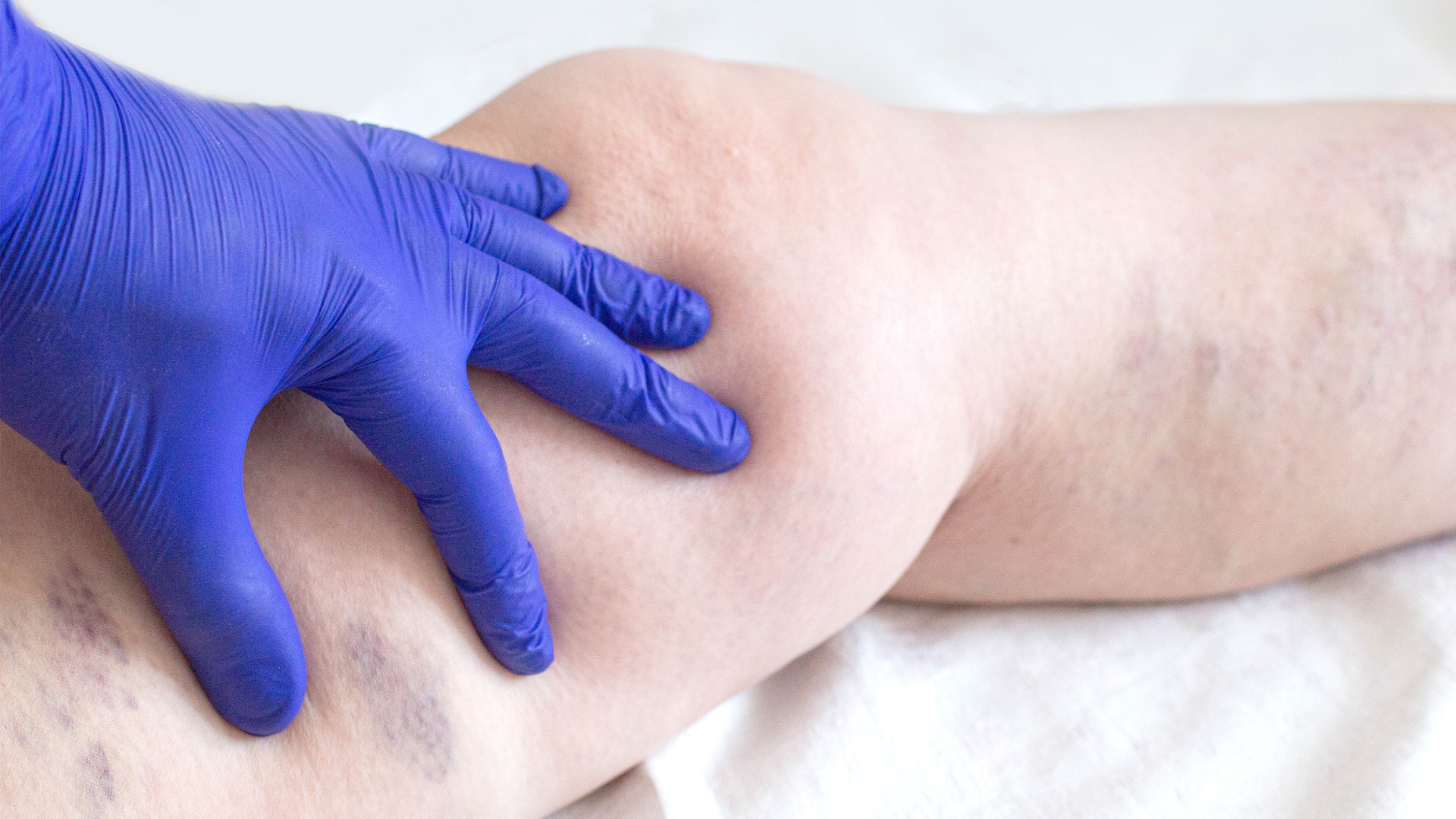
Do you or a loved one have mysterious sores on your legs?
Maybe the sores have formed right around the ankles.
They might hurt, and there might also be some swelling, some itching, or some oozing…
If this sounds familiar, and especially if you or a family member have a vein disease diagnosis such as venous insufficiency or varicose veins, keep reading, as we might have the answer for you.
In this article, we’re going to talk about one of the most difficult and uncomfortable conditions related to your veins: venous ulcers.
Venous ulcers, sometimes called leg ulcers, occur in up to 3 in 1000 people, and it is much more common in older patients[1]
And this condition is stubborn! Only 60% of these ulcers are healed after 12 weeks, and, after healing, 75% will experience a recurrence of ulcers within three weeks.[2]
This condition can be painful and debilitating and it affects not only the physical health but also the mental health of millions worldwide.
Let’s dive in and learn more about venous ulcers – their causes, symptoms, diagnoses, and treatment options.
Table of Contents
ToggleWhat are Venous Ulcers?
Venous ulcers are sores that happen when there is poor circulation of blood in your veins, particularly in your legs. [3]
Sometimes called venous stasis ulcers or varicose ulcers, these result from venous insufficiency, which is when the valves in your veins have trouble returning blood to your heart. The blood then backs up in the veins, pooling blood in the lower legs.
The continuous buildup of fluid leads to pressure, which then causes ulcers to develop. They typically occur on the leg above the ankle.[3]
Several factors can cause venous ulcers, which you can learn more about in the next section.
What causes venous ulcers?
So venous insufficiency is what causes these painful wounds to develop, but what causes the insufficiency in the first place?
Here are the most common behaviors or lifestyle factors associated with leg ulcers:
Prolonged sitting or standing. Staying in one position for too long can hinder blood circulation in your legs, whether you’re on your feet all day or sitting in an office chair for hours at a time.[6]
Obesity. Extra weight means extra pressure on your legs, including the veins, which can lead to venous insufficiency down the road.[4]
Age. Bodies change as we age, and that includes our veins. Vein structure can change over time, leading to changes in blood flow. This condition most often occurs in those over the age of 55.[4]
Family history. If your parents or grandparents have venous ulcers or have been diagnosed with vein disease, there is a stronger chance that you will too. There may be a genetic tie to this condition.[6]
Previous injury. If you’ve injured your legs or have needed leg surgery at some point, you may have damaged your veins as well, causing impaired blood flow, and leading to vein problems.[4]
Pregnancy. Like aging, pregnancy comes with many changes to the body, veins included. Hormonal changes and the growing uterus can lead to increased pressure in your legs and possible venous insufficiency.[6]
As you can see, certain causes are preventable. But others… not so much.
For some patients, certain kinds of venous disease are connected to chronic venous insufficiency and can exacerbate venous ulcers.
One example is deep vein thrombosis (DVT). Those experiencing DVT develop blood clots in the deep veins of their legs, which obstruct blood flow and lead to pressure and, eventually, damage to your veins. [4]
Another condition related to venous insufficiency is varicose veins. These are swollen, enlarged veins that are near the surface of the skin. They typically occur in the legs and often look blue or purple. They appear when veins become weak or damaged. [5]
While you can experience chronic venous insufficiency without the presence of varicose veins, many people deal with both simultaneously.
While there are many ways that this condition can develop, there are also many different ways to experience venous ulcers.
In the next section, we will discuss all of the different symptoms associated with leg ulcers.
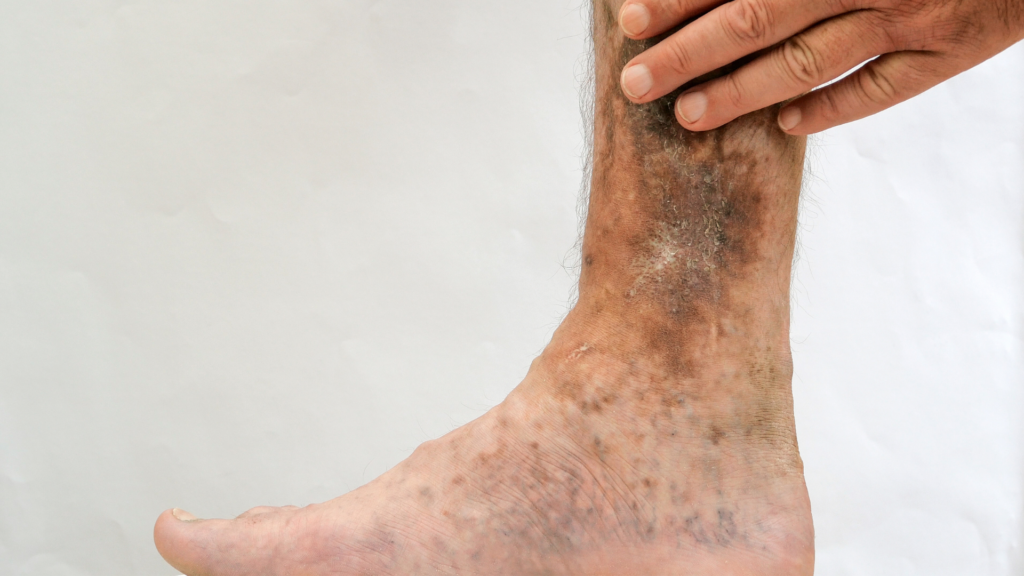
Venous Ulcers Symptoms
In simplest terms, venous ulcers are sores on the lower legs or ankles.
However, each person with this condition can feel varying levels of pain and uncomfortableness.
Like all sores, venous ulcers come with a variety of side effects, such as:[7]
Pain. Pain is a common side effect of venous ulcers, and additional inflammation or an infection can cause the pain to worsen.
Itching. Ulcers can feel itchy or irritating at times, especially as they are healing.
Swelling. While more a side effect of vein disease in general, many patients with venous ulcers can experience swelling, or edema, in their legs.
Discoloration. The discoloration, called hemosiderin deposition, stems from the breakdown of red blood cells, which can make skin near the ulcers appear reddish-brown.[8]
Drainage. Sores may produce a clear, yellow, or greenish-looking discharge. One should pay attention if they notice this, as it could be a sign that the venous ulcers are infected.
Another unfortunate side effect of this condition? These ulcers often take a long time to heal due to poor circulation that stems from venous insufficiency…[9]
Yes, the same insufficiency that caused them to appear in the first place!
That’s why it’s important to get to the root of the problem and seek treatment, which we’ll cover later on in this article.
But if you suspect you are experiencing venous ulcers, you’ll first need to get a diagnosis. Read on to learn about the diagnosis process.
Venous Ulcer Diagnosis
If you believe you are dealing with venous ulcers, you’ll want to make an appointment with your doctor.
There are then several steps they will take to confirm if you are suffering from this condition.[10]
- Review your medical history.
First things first, your doctor will look over your medical history and ask you questions about your symptoms, family history (particularly with vein disease), and day-to-day lifestyle to look further into the root cause of the ailment.
- Perform a physical exam.
Your doctor will then inspect your legs to look for clues that you may have venous insufficiency and ulcers. They’ll assess the characteristics of any wounds: size, depth, drainage, and any other skin changes.
- Order a Doppler ultrasound.
If your doctor suspects that you have venous disease, they may order a Doppler ultrasound to further assess your blood flow in your legs. This is a non-invasive imaging test that uses sound waves to generate images showing the flow of blood, which can identify the location and severity of any vein problems.
- Order additional testing.
If the doctor needs to rule out any other ailments or identify other related medical concerns, they may request further testing of you. For example, diabetes can impede wound healing, so they may order a blood test to determine if you have diabetes as well.
Once your doctor has gone through these steps above, they may be able to provide a venous ulcers diagnosis.
When you have received your diagnosis, it’s time to turn to treatment options. Keep reading to learn about the different treatment options available.
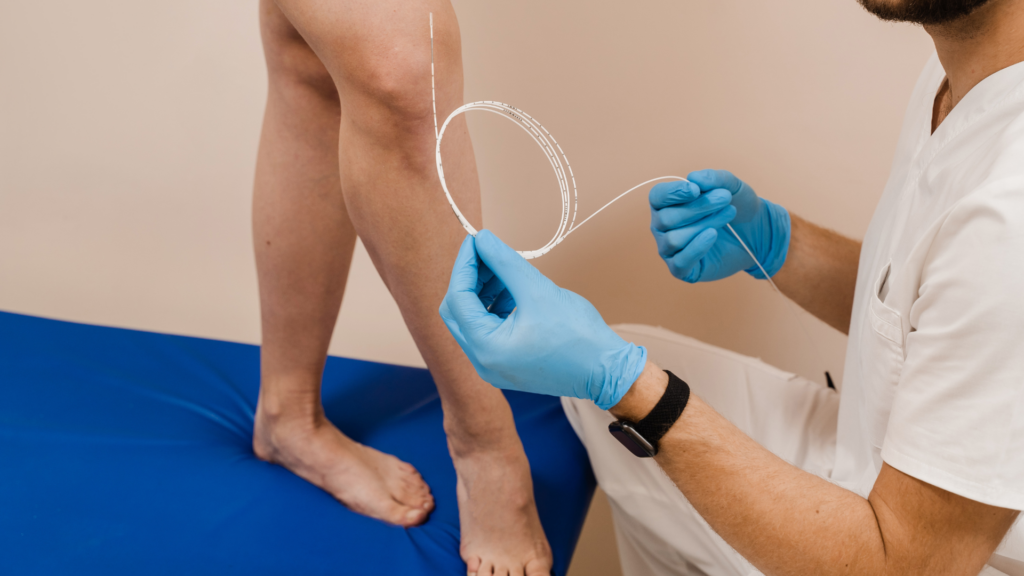
Medical Treatment for Venous Ulcers
As we’ve mentioned earlier in this article, the best way that you can conquer your venous ulcers is to take care of the underlying problem: venous insufficiency.
Your doctor will likely recommend medical treatment options focused on healing venous disease, which will hopefully cause the venous ulcer concern to subside as well.
However, it is important to provide care for the ulcers themselves to prevent the condition from worsening. [11]
Wound care.
Ulcers should be treated like any other wounds on the body. Your doctor may recommend cleaning the ulcer with a saline solution or trying certain topical treatments, and dressing wounds with bandages to promote healing and prevent infection.
Reducing moisture levels and cleaning the area.
Make sure the skin stays clean and dry to avoid ulcer complications. If you do use a moisturizer, avoid the ingredients lanolin, neomycin, and nickel.[7]
Medications for pain management.
Venous ulcers can be irritating, and when they become inflamed or infected, they can become quite painful. Over-the-counter pain relievers or certain topical creams can help.[12]
To tackle the root of the problem, you’ll want to turn to treatments for vein disease.
The following treatments tackle venous insufficiency to reduce symptoms and improve blood flow in your veins:
Compression therapy.
When practicing compression therapy, the patient will wear compression stockings that apply pressure to the legs. This helps the blood travel back upward and reduces swelling.[13]
Many different compression stocking options exist, each with its own strength and style. Your doctor may recommend a certain type of garment after assessing your current condition.
Radiofrequency ablation.
Sometimes called RFA, radiofrequency ablation is a minimally invasive procedure that uses radio waves to target problematic veins. Heat is used to seal varicose veins shut, which then directs blood flow to healthier veins.
This is a procedure best performed early on to help improve healing and decrease recurrence rates. [14]
Sclerotherapy.
This is another minimally invasive procedure, though often used for cosmetic purposes, where a solution is injected into affected veins to cause them to collapse. Sclerotherapy can improve symptoms of venous insufficiency in some patients.[15]
Vein surgery.
When there is a severe case of venous insufficiency or a patient has complications with their leg ulcers, a doctor may recommend surgery to repair or remove certain veins. [16]
Each patient’s experience with venous ulcers is different, so your doctor may recommend one treatment over the other depending on your condition.
But if you or a loved one are suffering from the effects of venous insufficiency, there are several treatment options out there to reduce symptoms or the recurrence of ulcers themselves.
In addition to treatment, there are habits one can take to reduce side effects or prevent ulcers altogether.
Keep reading to learn more about prevention methods, many of which can serve as additional ways to reduce pain from leg ulcers.
Preventing and Reducing Venous Ulcers
There are numerous lifestyle changes that you can implement to not only lessen the severity of venous insufficiency and venous ulcers but also prevent these conditions in the first place.
Here are some prevention tactics that you can try out to reduce your chances of developing venous ulcers.[17]
Move – and elevate – your legs.
When it comes to vein health, it’s not a good idea to sit or stand for too long. If you’ve done one or the other, take some time to kick your legs up for a bit. Maybe even try elevating them against a wall every so often or trying a yoga move that gets your legs up in the air.
Manage your weight.
Every extra pound is an extra pound sitting on your legs, increasing pressure and impeding blood flow. Instill healthy habits early on to help prevent venous disease later on.
Eat a healthy diet.
Support overall vascular health by eating a diet rich in fruits, vegetables, whole grains, and lean proteins. If you have an elevated risk for vein conditions, consider limiting your sodium intake, as this can lead to fluid retention and leg swelling.
Avoid smoking.
There are many health-related reasons to avoid cigarettes, and your vein health is included! Smoking can constrict your blood vessels and impair circulation, which can lead to venous insufficiency down the line. Quitting smoking or avoiding it altogether can greatly improve vascular health.
Stay active.
Move those legs! Aim for 150 minutes of exercise a week to reduce your risk of developing venous ulcers. Walking, swimming, and cycling are some activities that can improve blood circulation in your legs.
Find an emotional outlet.
For those actively suffering from leg ulcers, having an outlet for your feelings is crucial. As sores are visible on the skin, those with the condition may feel embarrassed, and the daily pain from the wounds can be exhausting. Talk to a family member or friend, journal, or meditate – build your support system.
Whether it’s the management of venous ulcers or preventing them altogether, these are all healthy habits that you should implement.
Conclusion
Venous ulcers may not be the most familiar of vein conditions.
However, It’s important to shed light on this condition that causes debilitating pain and discomfort for many people.
After reading this article, you’ve made yourself familiar with each part of this condition: causes, treatment, diagnosis, and prevention.
There is a very real chance that someone in your own life experiences venous insufficiency. And as you’ve learned, it’s not just about the physical toll, but the mental toll as well.
Understanding venous ulcers is not simply about expanding your knowledge, but also about taking control of your health and well-being and being able to support those around you.
By being able to identify the signs of venous ulcers and when to seek medical treatment and adopt lifestyle changes, you can prevent further medical trouble and improve your quality of life overall.
If you or a loved one are suffering from venous ulcers and feel pain and discomfort every day, there is help out there for you.
The team of experts at Elite Vein Clinic is here to provide solutions for vein conditions of all kinds. Our clinic is professional and patient-focused, providing top-of-the-line care and modern treatments for those experiencing a variety of vein-related medical concerns.
Take the first steps toward conquering your venous ulcers. Contact Elite Vein Clinic today!
References
- Nelson, E. A., & Adderley, U. (2016). Venous leg ulcers. BMJ Clinical Evidence, 2016. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4714578/
- Probst, S., Weller, C. D., Bobbink, P., Saini, C., Pugliese, M., Skinner, M. B., & Gethin, G. (2021). Prevalence and incidence of venous leg ulcers—A protocol for a systematic review. Systematic Reviews, 10. https://doi.org/10.1186/s13643-021-01697-3
- https://medlineplus.gov/ency/patientinstructions/000744.htm
- https://www.nhs.uk/conditions/leg-ulcer/causes/
- https://www.templehealth.org/services/conditions/varicose-veins-chronic-venous-insufficiency
- https://www.nyp.org/vascular/venous-insufficiency-and-ulcers
- https://www.cedars-sinai.org/health-library/diseases-and-conditions/v/venous-ulcers.html
- Caggiati A, Rosi C, Casini A, Cirenza M, Petrozza V, Acconcia MC, Zamboni P. Skin iron deposition characterises lipodermatosclerosis and leg ulcer. Eur J Vasc Endovasc Surg. 2010 Dec;40(6):777-82. doi: 10.1016/j.ejvs.2010.08.015. Epub 2010 Sep 28. PMID: 20880725.
- Raffetto, J. D., Ligi, D., Maniscalco, R., Khalil, R. A., & Mannello, F. (2021). Why Venous Leg Ulcers Have Difficulty Healing: Overview on Pathophysiology, Clinical Consequences, and Treatment. Journal of Clinical Medicine, 10(1). https://doi.org/10.3390/jcm10010029
- https://www.nhs.uk/conditions/leg-ulcer/diagnosis/
- Dogra, S., & Rai, R. (2014). Venous leg ulcer: Topical treatment, dressings and surgical debridement. Indian Dermatology Online Journal, 5(3), 371-373. https://doi.org/10.4103/2229-5178.137820
- Imbernon-Moya A, Ortiz-de Frutos FJ, Sanjuan-Alvarez M, Portero-Sanchez I, Merinero-Palomares R, Alcazar V. Pain and analgesic drugs in chronic venous ulcers with topical sevoflurane use. J Vasc Surg. 2018 Sep;68(3):830-835. doi: 10.1016/j.jvs.2017.11.071. Epub 2018 Feb 13. PMID: 29452834.
- Patton, D., Avsar, P., Sayeh, A., Budri, A., Walsh, S., Nugent, L., Harkin, D., Cayce, J., Corcoran, M., Gaztambide, M., & Moore, Z. (2023). A meta‐review of the impact of compression therapy on venous leg ulcer healing. International Wound Journal, 20(2), 430-447. https://doi.org/10.1111/iwj.13891
- Bonkemeyer Millan S, Gan R, Townsend PE. Venous Ulcers: Diagnosis and Treatment. Am Fam Physician. 2019 Sep 1;100(5):298-305. PMID: 31478635.
- Worthington-Kirsch, R. L. (2005). Injection Sclerotherapy. Seminars in Interventional Radiology, 22(3), 209-217. https://doi.org/10.1055/s-2005-921954
- https://nyulangone.org/conditions/chronic-venous-insufficiency/treatments/surgery-for-chronic-venous-insufficiency
- Shenoy, M. M. (2014). Prevention of venous leg ulcer recurrence. Indian Dermatology Online Journal, 5(3), 386-389. https://doi.org/10.4103/2229-5178.137824